Severe nausea and vomiting during pregnancy can cross a line where rest, ginger tea, and crackers are no longer enough. For women whose Hyperemesis Gravidarum otherwise known as HG signature line frequently results in a hospital. Coming to terms with what the term HG implies in a medical environment, when hospital care is required, and what occurs when you arrive hopefully takes some of the fright out of it.
In the rest of this guide, ‘HG’ means Hyperemesis Gravidarum a severe form of vomiting in pregnancy severe enough to require hospital admission not hospital names that happen to contain the initials h and g. This article aims to make other pregnant women fully aware of if and when hospital treatment for HG is necessary, and what to expect during and after admission.
Key Takeaways
- HG (Hyperemesis Gravidarum) defined as continual, excessive emesis, uncontrollable over and above normal morning sickness of pregnancy.
- You need to go into hospital for care if you‘re unable to keep fluids down for a period of hours, if you‘re dehydrated for example if your urine is very dark or you‘re feeling very faint and if you‘ve lost a noticeable amount of weight within a comparatively short period of time.
- Hospital management largely involves IV fluid rehydration, anti-meticetic drugs, and in some cases nutritional support.
- Most patients get better within a few days of being in the hospital, and they leave with a plan for medications, doctors’ visits, and continued home care.
- Acting early reduces risk — do not wait until you feel faint or notice very dark urine
What Is HG? (Hyperemesis Gravidarum Explained)
Hyperemesis Gravidarum (HG) is a complication in pregnancy, and is associated with continuous, profound nausea and vomiting. This results in dehydration, depletion of essential ions and significant. It is not an exacerbation of the typical nausea and vomiting of pregnancy it is a unique condition. The NHS definition of hyperemesis gravidarum states that the prevalence is 1 in 100 and is the commonest cause of hospital admission in early pregnancy.
Whereas ‘regular’ nausea of pregnancy usually peaks around weeks 6 to 9 and disappears by around week 12, HG can last well into the second trimester or even the whole pregnancy.
Dehydrate the woman of water and electrolytes faster than anyone even knows. It can harm mother and child when not treated.
HG vs. Normal Morning Sickness

HG is far more severe than typical morning sickness
| Feature |
Morning Sickness |
Hyperemesis Gravidarum (HG) |
| Nausea frequency |
Occasional, usually morning |
Persistent, often all day |
| Vomiting episodes |
Few times per day |
Multiple times per day, uncontrollable |
| Ability to keep fluids down |
Yes, mostly |
No — fluids are frequently lost |
| Weight loss |
Minimal or none |
More than 5% of pre-pregnancy weight |
| Impact on daily life |
Manageable with rest |
Severely debilitating |
| Hospital care needed |
Rarely |
Frequently required |
| Duration |
Usually resolves by week 12 |
Can last into second or third trimester |
Healthcare providers can also use the Pregancy-Unique Quantification of Emesis (PUQE) score to describe severity of nausea and vomiting within a 24 hour window. If PUQE is elevated, it indicates more significant symptoms, justifying closer observation or hospitalisation though this decision rests with your clinician while taking your general condition and pregnancy into account.
Warning Signs That Mean You Need Hospital Care for HG

Dehydration and weakness are key signs that need urgent care
Here is where many people wait too long. The symptoms below are not signs to “push through” — they are signals that your body needs medical support.
Seek hospital care if you experienceanyof the following:
- You haven‘t been able to keep anything down for many hours, and it is obviously getting worse rather than better.
- Your urine isdark yellow, orange, or brown a sign of dehydration)
- You are urinating much less frequently than normal (less than 3 times in 24 hours)
- You‘ve lost about 5% or more of your body weight before pregnancy or your clothes feel much looser in a short space of time.
- You get dizzy or you feel faint or lightheaded when you stand up
- Present with blood in your vomit
- You feel confused, extremely weak, or have a rapid heartbeat
- You have a high fever alongside vomiting
You do not have to check every box. Just one or two of these symptoms have to be present in order for you to have it checked out immediately.
When to Call Your Doctor vs. When to Go to the ER
Call your OB or midwife first if:
- Symptoms are worsening over several days but you can still keep small amounts of water down
- You have lost some weight but are not displaying acute dehydration signs
- You want guidance before presenting to a hospital
Go directly to the emergency department if:
- You cannot stand without dizziness
- There is blood in your vomit
- Since you last urinated, it has been time.
- You are feeling very confused, or you are experiencing chest pain along with vomiting.
Do not try to drive yourself. Get someone else to take you or contact emergency services if you think you can’t keep standing without risking injury.
What Hospital Treatment for HG Looks Like
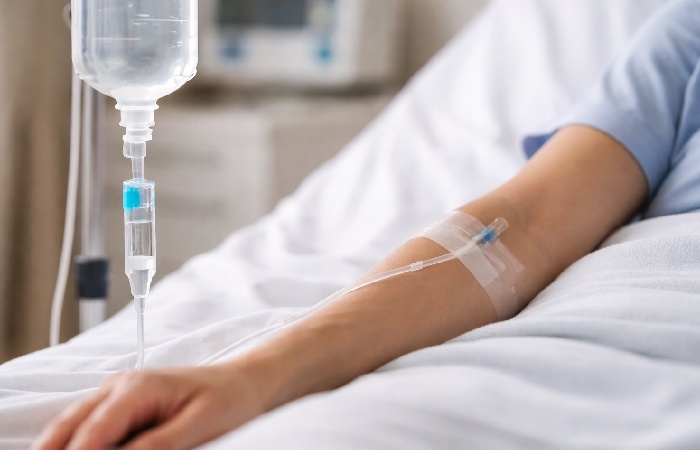
IV fluids help restore hydration and electrolytes quickly
According to the Cleveland Clinic‘s summary of HG treatment, the main aim of inpatient management of HG is to rehydrate, halting the vomiting cycle and re-establishing nutritional equilibrium. Treatment is thus tailored according to severity of symptoms.
Intravenous (IV) Fluids and Rehydration
First, you need to put back what you‘ve lost, in the form of fluids and electrolytes. You will be given a drip (call an IV line), usually in your arm. This will deliver saline and electrolytes (sometimes glucose) to your blood directly.
This alternative eliminates the need to pass through the digestive system and therefore is effective even for patients who are unable to keep anything down. Full effects, such as relief from dehydration symptoms, are typically felt within the first 12-24 hours of IV therapy.
Antiemetic Medications Used in Hospital
When re-hydration is resumed, the care team will treat the vomiting. Since many patients are unable to absorb medications, anti-emetics are frequently given parenterally.
Commonly used medications include:
- Ondansetron (Zofran) a popular antiemetic but the use in early pregnancy is discussed with a great deal of caution; the benefits and risks are taken into account by your practitioner
- Metocidogramide- prevents nausea and facilitates gastric emptying
- Promethazine for severe nausea; may cause drowsiness
- (Pyridoxine Vitamin B 6) sometimes combined with doxylamine as first-line treatment.
As relates to medication safety in pregnancy: the FDA info about anti-emetics in pregnancy gives a listing of what is approved. They will decide based on the gestational age, severity of nausea, your past risk factors. Have your team of providers explain to you the reason for any medications you are prescribed.
Nutritional Support for Severe Cases
When vomiting is extreme and prolonged — and especially when weight loss is significant — the body cannot meet its caloric and nutritional needs through normal eating. In these cases, two approaches may be used:
Nasogastric (NG) tube feeding: A thin, flexible tube is passed through the nose into the stomach, delivering liquid nutrition continuously. This is uncomfortable but is tolerated well by many patients once they adjust.
Total Parenteral Nutrition (TPN): In extreme cases, the provision of nutrients is directly provided by a central intravenous (IV) line and the gut is entirely avoided. TPN is a method of last resort and used in circumstances in which a patient is unable to undertake some level of enteral Nutrition.
Both approaches are temporary. The goal is always to return to normal eating as soon as symptoms allow.
Preparing for a Hospital Stay With HG
If you know — or strongly suspect — that hospital care is coming, a little preparation reduces stress.
What to Bring and Expect on Admission
- Please bring your pregnancy notes / medical card and a list of any medication you are currently taking.
- Wear loose, comfortable clothes (an IV may be in the arm)
- Charge your phone; the sitings, as they are called, can be anywhere from 1 day to many days
- Mention allergies to the admissions team. List all known allergies (especially to medications)
- Let someone know you‘re going in, so you will be supported
When you arrive you probably will be weighed, have bloods taken to see how your electrolytes and kidneys are, and a sample of urine tested for ketones (a sign you are lacking in nutrition). An ultrasound may be done to see how the pregnancy is going.
Questions to Ask Your Care Team
- What medications do you advise and on what grounds?
- What are the advantages and disadvantages of each ‘treatment’ for my stage of pregnancy?
- What way do you have to choose when I‘m good to go home?
- What if I find I am feeling worse after I leave hospital?
You should get straightforward answers to each of these questions. If someone on the team has trouble explaining in simple terms why you are being treated a particular way, ask again or call your OB.
After Discharge — What Comes Next
HG in hospital does not cure but controls the HG. Quite a few patients go back home with a bit of nausea – but under control.
Home Management and Follow-Up Care
Your discharge plan will typically include:
- Prescription for oral antiemetics to be used at home
- Advice for foods; avoid hot and irritating foods such as irritating spices; fats, meats and alcohol; advise to eat something before taking the medication. Small, frequent meals; eat cold or room temp foods; avoid strong smells.
- A review within 3–7 days
- Explicit information regarding when should you go back to hospital or contact your provider
Follow-up is not elective. HG can return quickly in the first trimester. Make sure you keep your follow-up appointment even if you are feeling much improved.
At home:
- Sip small amounts of fluids frequently instead of drinking large quantities at one time
- Rest where you are as much as you can as fatigue increases the feeling of nausea.
- Lean on family or a support network; HG is not something you should deal with on your own.
HG and Your Mental Health
HG is physically exhausting. It is also isolating, particularly in early pregnancy when many women have not yet shared the news. It‘s common for women with HG to feel depressed, anxious or helpless and these aren‘t a sign of weakness, but real problems that need treatment.
If your HG experience (whether during or after a hospital admission) is making you upset, don‘t be afraid to tell your medical team. Your recovery plan may include some support from a specialist mental health service. You do not only need your levels checked you deserve all the support you need.
Common Mistakes With HG Hospital Care
Many women with HG wait too long to seek hospital care because they hope things will improve on their own or feel guilty about “making a fuss.” Leaving it late often means you arrive more dehydrated and need a longer recovery. An all too common problem is if you‘re discharged from hospital before you can reliably keep down fluids and your medications which will make it more likely you‘ll be readmitted within a day or two. Adhering to the discharge plan and attending your follow-up appointment are part of treatment.
Who This Guide Is For / Who Should Seek Care Immediately
This guide is most useful for:
- Nausea and Vomiting of Pregnany who have persistent nausea and vomiting and who‘s symptoms they cannot decide.
- Family members or partners seeking information on the condition and what to expect
- Anyone who has been told they may need hospital admission for HG and wants to be prepared
Seek medical care immediately — do not wait — if:
- You have not kept any fluid down for many hours and are feeling weaker, dizzier, or more unwell as time passes
- You feel faint, confused, or have blood in your vomit
- You have not urinated in many hours
Note: HG is a YMYL (your health and your life) topic. All content contained in this article is for educational purposes only, it should not be used as a substitute for a direct discussion with your obstetrician, midwife, or emergency physician. Every pregnancy differs and one can only make treatment decisions with a health care provider who is familiar with your complete medical history.
Frequently Asked Questions
Q: When should I go to the hospital for HG?
A: Seek medical help if you are unable to retain fluids at all for an extended period, your urine becomes dark or you urinate significantly less than normal, you feel extremely light-headed when standing up, or you‘ve experienced a rapid weight-loss. It is advisable to attend early before the condition becomes severe, as this will be more easily treatable and may also limit further problems.
Q: How long does a hospital stay for HG typically last?
A: Lengths of hospital stay vary. Most women stay for a few days depending on how quickly they respond to IV fluids and anti-emetics. Severe or complicated hyperemesis will take longer and may result in repeat hospital stays. You will normally be discharged once you are able to tolerate some oral fluids, your blood tests and observations are stable.
Q: Is HG dangerous for the baby?
A: In most HG cases, the pregnancy will still be safe. This is even more true if help is sought early. Extensive, undiagnosed protracted severe HG( with considerable malnutrition) can be dangerous. This is one of the main reasons admission is advised once symptoms reach a certain level. Your OB will be monitoring foetal wellbeing during and after admission.
Q: Can HG come back after a hospital stay?
A: yes certainly HG can relapse, especially in the first trimester. As I mentioned before, discharge does not mean you are no longer sick, rather it means you have been brought down to a safer level. Keep with your discharge plan, see your doctor as scheduled and if you are feeling worse, then call your provider.
Q: Is there a difference between HG hospital and a normal maternity hospital?
A: Any hospital where the care of HG is provided is called HG hospital. A hospital/clinic/center/unit is NOT called HG hospital. It just means the payer‘s facility covered the cost of care for HG. If you want to know the specific HG hospital, then find out the names of hospitals in your region, for example, in India, go to local yellow pages and contact the state health dept.