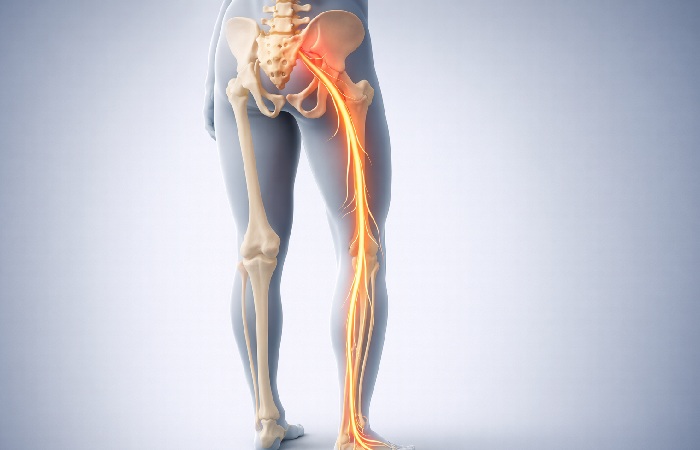
Pain from your sciatic nerve does more than hurt. It burns, shoots and radiates down your leg in a way that makes it difficult to sit, stand or lie down. That‘s probably why you‘re here.
The good news: a 10-minute sequence of natural movements and stretches, focused on the affected area, can make a real difference if you perform it correctly. The not-so-good-news: 10-minutes of targeted stretches and movements won‘t be enough to completely heal your sciatica. It will, however, break the pain-spasm cycle, loosen the muscles pinching the nerve, and create an environment in which your body can begin to heal.
This guide discusses just how to do that, how to determine if it‘s effective, what not to do, and when self-care alone won‘t be sufficient.
Note: There is no intent to offer medical advice from this article. Please see your qualified practitionar when seeking diagnosis and treatment for any medical problem.
Quick Answers Before We Begin
- What is sciatica?->Pressure on or irritation of the sciatic nerve, resulting in pain that radiates from the back of your lower limb, through your hips and down the thigh to the leg.
- Sure, is a 10 minute routine really going to work? -> Definitely, for a lot of people doing a few targeted stretches can relieve pressure on the nerve from tight muscles and be a temporary but genuine cure.
- How do I know the exercises are working?-> Any pain should be movingtoward your back (centralize), not lower down your leg.
- When do I finish right now?-> If pain gets worse, goes into both legs or you feel numbness/tingling intensify.
- When should I visit a doctor?-> If symptoms are severe, have not settled after 3–4 weeks or you develop loss of control of any bladder or bowels.
What Is Sciatica — And Why Does It Hurt So Much?
Sciatica isn‘t a condition. It describes a collection of symptoms that occur when the sciatic nerve is compressed or irritatedthe sciatic nerve is the longest in the body, running from your lower back, through your buttocks and hips and down to the foot on either leg. According to the Mayo Clinic, sciatica only affects one side of the body at a time and pain can vary from a slight burning to a sharp pain.
A nerve gets jammed, pinched or inflamed, the pain starts to travel up and down the course of the nerve itself. That is the feeling we experience as sciatic pain anywhere from your lower back to your calf, and commonly as a burning or electric shock sensation rather than muscle pain.
The Sciatic Nerve: A Quick Anatomy Note
The sciatic nerve is derived from nerve roots from the lumbar vertebrae L4, L5 as well as the sacral segments S1–S3 it leaves the spinal column, enters through the pelvis and posterior to the piriformis muscle, before coursing down the back of the thigh. The NIH‘s StatPearls with regard to sciatica describes it as the longests, widest nerve in the human body that is why effects of compression anywhere along its pathway can cause such widespread symptoms.
This pathway matters because the source of compression determines which movements help — and which ones can make things worse.
Common Causes of Sciatic Nerve Compression
- Herniated (bulging) disc Cause found in approximately 90% of cases, according to NIH/NCBI research of lumbar disc herniation. A disc between vertebrae protrudes and compresses on a nerve root.
- Piriformis syndrome — The piriformis muscle in the buttock tightens or spasms, compressing the sciatic nerve from the outside. Research published via NCBI’s StatPearls on piriformis syndrome estimates this accounts for up to 6% of sciatica presentations.
- Spinal stenosis- narrowing of the Spinal canal. More common in those over 50.
- Degenerative disc disease (This is aging disc degeneration weakening cushioning between vertebrae).
- Pregnancy The gravid uterus has the potential to irritate the sciatic nerve, especially in the third trimester.
- Sitting for long periods Continuous compression of the piriformis due to long hours sitting on firm surfaces the nerve over a period of time.
Why this matters for your routine: As the Cleveland Clinic notes on sciatica, herniated disc sciatica and piriformis syndrome often require different treatment approaches. Some stretches that relieve one tend to worsen the other. While those available in this guide should be safe for most, if you have a specific condition, ask a physical therapist about an individualized routine..
The Honest Truth About “10-Minute” Sciatic Relief
Here’s where a lot of “quick fix” content misses the mark — and where we’ll be straight with you.
A 10-minute movement routine can:
- Reduce muscle tension pressing on the nerve
- Improve blood flow to inflamed tissue
- Encourage the sciatic nerve to glide more freely through its pathway
- Provide meaningful short- to medium-term pain reduction
A 10-minute routine cannot:
- Repair a herniated disc
- Reverse spinal stenosis
- Replace physical therapy for a structural problem
The centralization principle — your built-in progress indicator:
There‘s a clinical concept called centralization in physical therapy. Pain moving away from your leg and toward your low back when you perform the “correct exercises” is actually a good thing. It indicates that a nerve is being decompressed.
If pain moves further down your leg during or after a stretch, that’s peripheralization — a signal the movement may be increasing compression. Stop that stretch and try a different one.
Use this as your real-time feedback mechanism. It takes the guesswork out of whether these exercises are helping or hurting.
The 10-Minute Natural Sciatic Relief Routine
On a firm padded surface (yoga mat or carpeted floor). Do slowly. No physical force should be used. If any movement produces pins and needles, or rushes symptoms further down your leg – stop immediately.
This exercise is recommended to treat mild to moderate sciatic pain. If any of the aforementioned applies to you it is best to see a doctor or a physiotherapist before attempting this exercise: your pain is very excruciating, you have a verified disc herniation or you are experiencing neurological symptoms ( leg weakness/gland control).
Step 1 — Diaphragmatic Breathing (1 minute)
Lying on back, knees bent, feet flat. One hand on one hand on the belly one hand on the chest. Notice the magnitude of breath into your nose through the #. Only the belly should rise. Breath out for 6 counts.
Why: Deep breathing here is to calm your nervous system before you move. It also loosens tight deep hip and low-back muscles that might be causing your sciatic nerve compression.
Step 2 — Knee-to-Chest Stretch (2 minutes)
- From the same position, slowly draw one knee toward your chest.
- Hold your shin (not your knee joint) gently.
- Hold for 20–30 seconds. Feel a gentle release in the lower back and glute.
- Lower slowly. Repeat on the other side.
- Complete 3 repetitions per side.
Why: This position provides a mild decompression of the lower lumbar area and a streatching of the piriformis and gluts two of the more common compression sites for sciatica.
Centralization check: Does the pain move toward your back? Good. Does it move down your leg? Stop this stretch.
Step 3 — Figure-Four (Piriformis) Stretch (3 minutes)
This stretch targets the piriformis muscle, a common source of sciatic nerve compression
- Dr. lie on your back, knees bent.
- Cross your most-affected ankle over your opposite knee, forming a ‘4’.
- Okay now for the crossed leg ask your participant to flex the foot (or points toes to the shin of the crossed leg).
- Gently apply downward and inward pressure with your uncrossed thigh. Pull downwards and inward on the uncrossed thigh until you begin to feel a stretch deep within your buttock.
- Hold for 30–45 seconds, breathing gently all the time.
- Repeat 2–3 times per side.
Why: This is the most effective single stretch for piriformis syndrome and one of the most widely recommended for general sciatic compression. It directly targets the piriformis muscle and the deep hip rotators surrounding the sciatic nerve’s exit point.
Don’t force it. You should feel a deep, dull stretch in the buttock — not pain.
Step 4 — Cat-Cow Spinal Mobilization (2 minutes)
- Moved into a position on hands and knees, with wrists positioned directly beneath shoulders and knees directly below hips.
- Inhale: Shift the Comfortablynking belly toward theflor, lift your head and tailbone (Cow).
- Exhale: Curving spine up to celing, tuck chin and pelvis (Cat).
- Move slowly and in a rhythmic motion. Make 10–15 full cycles.
Why: Cat-Cow. Mobilises the whole of the lumbar spine, loosens off the painful joints that have become stiff, and promotes flowing movement around the disc and nerve root area. Gentle enough to be appropriate even with most disc and piriformis presentations.
Step 5 — Sciatic Nerve Glider / Nerve Floss (2 minutes)
- Sit up in a chair with your feet resting flat on the floor.
- Lightly straiten the knee of your affected leg to the point just short of forcing it straight.
- Simultaneously, dorsiflex foot (bring toes toward your shin).
- Hold for 2–3 seconds. Then slowly reverse back to the starting position.
- Repeat 10 15 times, slowly (not the way we normally do it but in a steady way).
Why: This is a nerve gliding (nerve flossing) exercise. Rather than stretching the nerve, it encourages the sciatic nerve to slide freely through its surrounding tissues, reducing neural tension and improving mobility. Nerve mobilization is a recognized component of conservative physiotherapy for lumbar radiculopathy, as referenced in NIH/NCBI literature on radicular back pain.
Important: This exercise should feel like a mild, tolerable stretch — not sharp pain. If symptoms worsen, stop.
Your 10-Minute Routine at a Glance
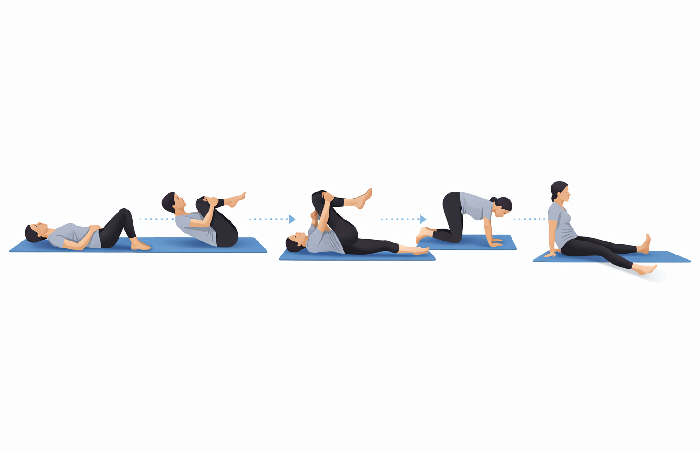
A simple sequence of movements to relieve sciatic nerve pressure
| Step |
Exercise |
Time |
| 1 |
Diaphragmatic Breathing |
1 min |
| 2 |
Knee-to-Chest Stretch |
2 min |
| 3 |
Figure-Four (Piriformis) Stretch |
3 min |
| 4 |
Cat-Cow Spinal Mobilization |
2 min |
| 5 |
Seated Nerve Glider |
2 min |
| Total |
|
10 minutes |
Perform once daily. Apply heat for 10–15 minutes beforehand. Stop any movement that causes pain to spread further down your leg.
Ice or Heat? What Actually Helps Sciatica
One of the most common questions — and one where getting it wrong can increase inflammation.
|
Ice (Cold Therapy) |
Heat Therapy |
| Best for |
Acute flare-ups, first 48–72 hours |
Chronic aches, muscle tightness |
| How it works |
Reduces inflammation; numbs acute pain |
Increases blood flow; relaxes tight muscles |
| How to apply |
Ice pack wrapped in cloth, 15–20 min |
Heating pad or warm towel, 15–20 min |
| Frequency |
Every 2–3 hours in acute phase |
Before stretching; for ongoing stiffness |
| Caution |
Never apply directly to skin |
Don’t fall asleep with heating pad on |
Harvard Health Publishing notes that most people with sciatica benefit from switching to heat once the initial acute inflammatory phase — typically the first 48–72 hours — has passed. Ice is more useful for numbing sharp, acute pain; heat helps relax muscle tightness that may be compressing the nerve.
Practical tip: Apply heat for 10–15 minutes before doing your relief routine to warm the muscles and make stretches more effective.
What NOT to Do — Common Mistakes That Make Sciatica Worse
Most of these are well-intentioned habits. That’s what makes them tricky.
- Bed rest for more than 1–2 days. The NHS advises that staying active is one of the most important things you can do for back and sciatic pain. Prolonged inactivity increases stiffness and can worsen nerve sensitization.
- Toe-touch forward bends. Forward bend with a rounded lower back leads to much greater disc pressure while aggravating herniation sciatica. This is very harmful in the setting of an acute flare up.
- Sitting on your wallet. A wallet or phone in your back pocket creates an imbalanced pelvis and compresses the piriformis — a surprisingly common trigger.
- Pushing through sharp or spreading pain. If a stretch causes pain to worsen or travel further down your leg, stop immediately — this is the peripheralization signal described above.
- Exercise while inflamed. Running, jumping or lifting heavy things while inflamed will worsen nerve compression.
- Forcing stretched positions. Aggressive stretching of an irritated nerve can cause micro-trauma. Gentle, sustained pressure is more effective than forcing a range of motion.
Beyond 10 Minutes — Sciatica-Proof Your Day
The 10-minute routine only helps if you’re not re-inflaming the nerve the other 23 hours and 50 minutes. Here’s how to integrate relief into your whole day.
For desk workers:
- Set a timer to interrupt sitting and get up and walk around every 45–60 minutes for 2–3 minutes. Sitting for extended periods of time is one of the most reliable sciatica aggravators, especially when symptoms are related to piriformis compression.
- Use a lumbar support pad. Or roll up a small towel to preserve the curve in your lower back.
- Both feet must be kept flat on the floor. CrosseD legs will tilt the pelvis downward and compress the piriformis.
Sleep position:
- Side laying with a pillow between the knees is probably the most comfortable position for your sciatic nerves this position maintains the hips in a neutral position and minimizes rotation of the spine.
- Positioning yourself on your back with a pillow under your knees will reduce stress on the lumbar spine.
- Stomach sleeping is the most discouraged of all positions for sciatic pain, since it promotes lumbar extension and can irritate nerve roots.
Posture micro-habits:
- When standing, distribute weight evenly between both feet. Habitually shifting all weight to one hip compresses that side’s piriformis.
- When lifting, bend your knees — never your back. The Mayo Clinic lists improper lifting mechanics as a recognized risk factor for developing sciatica.
Who This Routine Is For (And Who Should Avoid It)
Quick self-check — does this sound like you?
- Will a long 20+ minutes sit interval almost worsen your pain? -> More prone to piriformis associated compression. Concentrate on Step 1, 3 and 4.
- Does bending forward worse or cough suddenly? -> more reliable for disc-related sciatica. Less so for Steps 1, 2, and 4 and worry about Step 5.
This routine is appropriate for:
- Adults with mild to moderate sciatic pain, whether acute or recurring
- People with piriformis syndrome or muscle-tightness-related sciatic compression
- Desk workers experiencing sciatica from prolonged sitting
- Pregnant women (modified — skip the nerve glider; consult your OB/GYN first)
- People looking for a natural complement to existing physical therapy or medical treatment
Approach with caution or avoid without medical clearance:
- Patients with unequivocal severe disc herniation who have a profound leg weakness.
- Individuals with spinal instability, previous fusion, or fractures of the vertebrae
- Anyone with pain which is becoming worse quickly, both legs, or any associated neurological deficits (weakness, numbness, incontinence of bladder/bowel))
- Individuals who are role of the doctor to avoid certain movements
When in doubt, the right starting point is a physical therapist or physician — not a blog post.
When to See a Doctor — Red Flag Symptoms
Conservative self-care resolves a significant portion of sciatica cases. According to the Mayo Clinic, most people with sciatica improve within 4–6 weeks with rest, gentle movement, and appropriate over-the-counter anti-inflammatories — without the need for surgery.
Seek medical attention if:
- Pain has not improved after 4–6 weeks of consistent self-care
- The pain is severe, constant, or getting progressively worse
- You experience significant weakness in your leg (difficulty lifting your foot — “foot drop”)
- Numbness or tingling is spreading or worsening
- You have pain in both legs simultaneously
Seek emergency care immediately if:
- You lose control of your bladder or bowel function
- You develop saddle anesthesia (numbness in the groin and inner thighs)
These can be signs of cauda equina syndrome — a rare but serious spinal emergency. The Cleveland Clinic’s overview of cauda equina syndrome confirms that sudden loss of bladder or bowel control, combined with leg weakness or saddle numbness, requires immediate emergency medical assessment. Do not wait.
Frequently Asked Questions
Q: How quickly can I expect relief from these exercises?
A: Not for most, though most patients experience, on average, pain reduction in 1-3 sessions of practice and significant improvement from days to weeks.
Q: Can I do this routine every day?
Q: Yes, once per day would be sensible for most people do not undertake the routine at times of sharp pain, use ice initially to settle inflammation, then attempt movement as pain will allow.
Q: Will these exercises cure my sciatica?
A: Most likely not. This program aims to treat the symptoms and help you to recover and not to recover the structural causes – disc herniation, spinal stenosis. Consider this as part of your overall recovery plan, not the only solution.
Q: Is walking good for sciatic nerve pain?
A: In most cases, yes. Harvard Health Publishing recommends staying active and avoiding bed rest. Brief walks of 10–20 minutes can help reduce inflammation and keep up flexibility that can increase sciatica. Do not force walking through pinching, progressing pain.
Q: What’s the difference between sciatica and piriformis syndrome?
A: Both also cause a pain pattern which radiates down the leg, but the sites that causes pain differ. Classic sciatica, which is due to a herniated disc, is due to compression at the nerve root site within the spine, whereas in piriformis syndrome the compression site is outside the spine at the sciatic nerve, caused by the piriformis muscle. This point has been reviewed in NCBI‘s clinical literature on piriformis syndrome: this distinction is important not least because the two conditions have different treatment priorities and because some stretches may worsen either compressive issue.
Q: Should I use a TENS unit for sciatica?
A: TENS units are sometimes effective in the immediate management of pain in certain individuals. The evidence regarding the effectiveness of the TENS units for sciatica is inconsistent and they do not treat the cause of the pressure on the nerves. You should consult your Doctor before considering using one.
Final Takeaway
Sciatic nerve pain is a common condition, affecting between 10% and 40% of adults in their lifetime, as per the National Institutes of Health (NIH) – it need not take over your day.
It is normal for people to experience pain along their sciatic nerve at some point in their lives. Studies estimate between 10% and 40% of adults will endure sciatic nerve pain throughout the duration of their lives. Even though this is common, it does not mean you have to suffer through it day after day.
A 10-minute natural rest routine performed correctly and safely can deliver real results less pain, a greater range of motion and the body working to accelerate your natural ability to heal. The trick is doing the right exercise, listening to your body‘s response (translation: the centralization principle) and applying it to your lifestyle.
If your pain is extreme, structural, or persistent juts on your own, don‘t just stretch. A physical therapist or doctor can identify the precise reason and that‘s what to develop a plan around.
Begin gently. Remain faithful. And recognize when to call in reinforcements.
Medical Disclaimer:
About Healthbloomin